Allergies and intolerances are distinct physiological responses often confused due to overlapping symptoms. An allergy involves the immune system reacting to a harmless substance, potentially causing life-threatening anaphylaxis, whereas an intolerance is primarily a digestive issue resulting from the body’s inability to process specific food components or chemicals.
In the modern health landscape, the terms “allergy” and “intolerance” are frequently used interchangeably, yet they represent vastly different biological processes. Understanding the distinction is not merely a matter of semantics; it is a critical safety issue. While an intolerance can cause significant discomfort and distress, a severe allergy can be fatal within minutes. This comprehensive guide explores the mechanisms, symptoms, diagnostic procedures, and management strategies for both conditions, empowering you to navigate your health with authority.
The Fundamental Differences: Immune vs. Digestive Systems
The primary distinction between an allergy and an intolerance lies in the body system involved. This difference dictates the severity of the reaction and the necessary medical intervention.
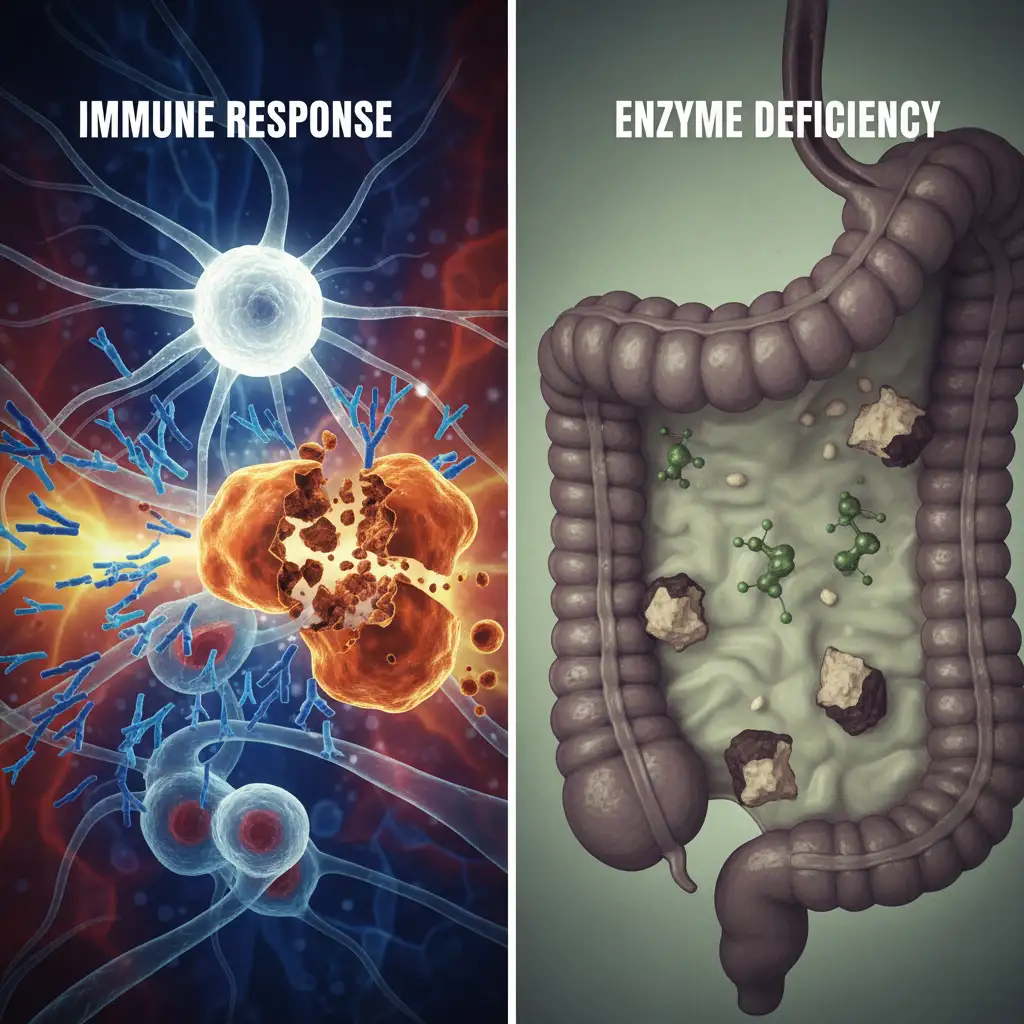
Food Allergy (Immune System): In a true food allergy, your immune system mistakes a specific food protein as a harmful pathogen. It produces antibodies called Immunoglobulin E (IgE) to fight this “invader.” When you consume the food again, these antibodies signal your immune system to release massive amounts of chemicals, including histamine, into your bloodstream. This chemical cascade causes the symptoms of an allergic reaction.
Food Intolerance (Digestive System): An intolerance generally occurs in the digestive tract. It is often caused by an enzyme deficiency, meaning the body lacks the specific enzyme required to break down a food component. For example, lactose intolerance is caused by a deficiency in lactase. Unlike allergies, intolerances are usually dose-dependent; a small amount of the offending food might be tolerated without symptoms.
Understanding Allergies: Triggers and Mechanisms
Allergies can range from mild seasonal nuisances to life-threatening emergencies. The prevalence of allergies has been rising globally, making awareness essential.
Common Food Allergens
While any food can theoretically cause an allergy, the vast majority of reactions are caused by the “Big 9” allergens:
- Milk: Common in children, often outgrown.
- Eggs: Specifically the proteins found in the white or yolk.
- Peanuts: One of the most common causes of severe anaphylaxis.
- Tree Nuts: Includes almonds, walnuts, cashews, and pistachios.
- Fish: Such as salmon, tuna, and cod.
- Shellfish: Crustaceans (shrimp, crab) and mollusks (clams, oysters).
- Soy: A common ingredient in processed foods.
- Wheat: Often confused with gluten intolerance, but involves an IgE response.
- Sesame: Recently added to the major allergen list in several jurisdictions.
Environmental and Drug Allergies
Allergies are not limited to food. Environmental triggers include pollen (hay fever), dust mites, mold spores, and pet dander. Drug allergies, such as reactions to penicillin or sulfa drugs, are also immune-mediated and can be severe.
Anaphylaxis: A Medical Emergency
The most severe form of allergic reaction is anaphylaxis. This is a rapid-onset, whole-body reaction that can impair breathing, cause a dramatic drop in blood pressure, and lead to unconsciousness. Immediate administration of epinephrine (adrenaline) is the only effective treatment for anaphylaxis. According to the American Academy of Allergy, Asthma & Immunology (AAAAI), delays in administering epinephrine are a major factor in fatal outcomes.
Food Intolerances Explained: Enzyme Deficiencies and Sensitivities
Intolerances are far more common than true allergies but are often more difficult to pinpoint because symptoms can be delayed, appearing hours or even days after consumption.
Lactose Intolerance
This is the most prevalent food intolerance globally. It occurs when the small intestine does not produce enough of the enzyme lactase to digest milk sugar (lactose). Undigested lactose moves into the colon where bacteria ferment it, producing gas, bloating, and diarrhea.
Histamine Intolerance
Some individuals have difficulty breaking down histamine, a chemical naturally present in foods like aged cheese, wine, and fermented products. This is often due to a deficiency in the diamine oxidase (DAO) enzyme. Symptoms can mimic allergies, including headaches, skin flushing, and nasal congestion.
FODMAPs and IBS
Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols (FODMAPs) are short-chain carbohydrates that are poorly absorbed in the small intestine. For people with Irritable Bowel Syndrome (IBS), these sugars can cause significant distress. A low-FODMAP diet is a clinically proven method to manage these symptoms.
Comparing Symptoms: How to Tell Them Apart
While there is overlap, the nature and timing of symptoms often provide clues to the underlying condition.
| Feature | Allergy (IgE-Mediated) | Intolerance (Non-IgE) |
|---|---|---|
| Onset Time | Immediate (minutes to 2 hours) | Delayed (hours to days) |
| Amount Triggering Reaction | Trace amounts can be fatal | Often dose-dependent (small amounts okay) |
| Primary Symptoms | Hives, swelling, wheezing, anaphylaxis | Bloating, gas, diarrhea, nausea |
| Life Threatening? | Yes (potential for anaphylaxis) | No (but affects quality of life) |
Diagnosis and Clinical Testing
Self-diagnosis is notoriously inaccurate in this field. Proper clinical testing is required to distinguish between allergies, intolerances, and other underlying conditions.
Skin Prick Tests and Blood Tests
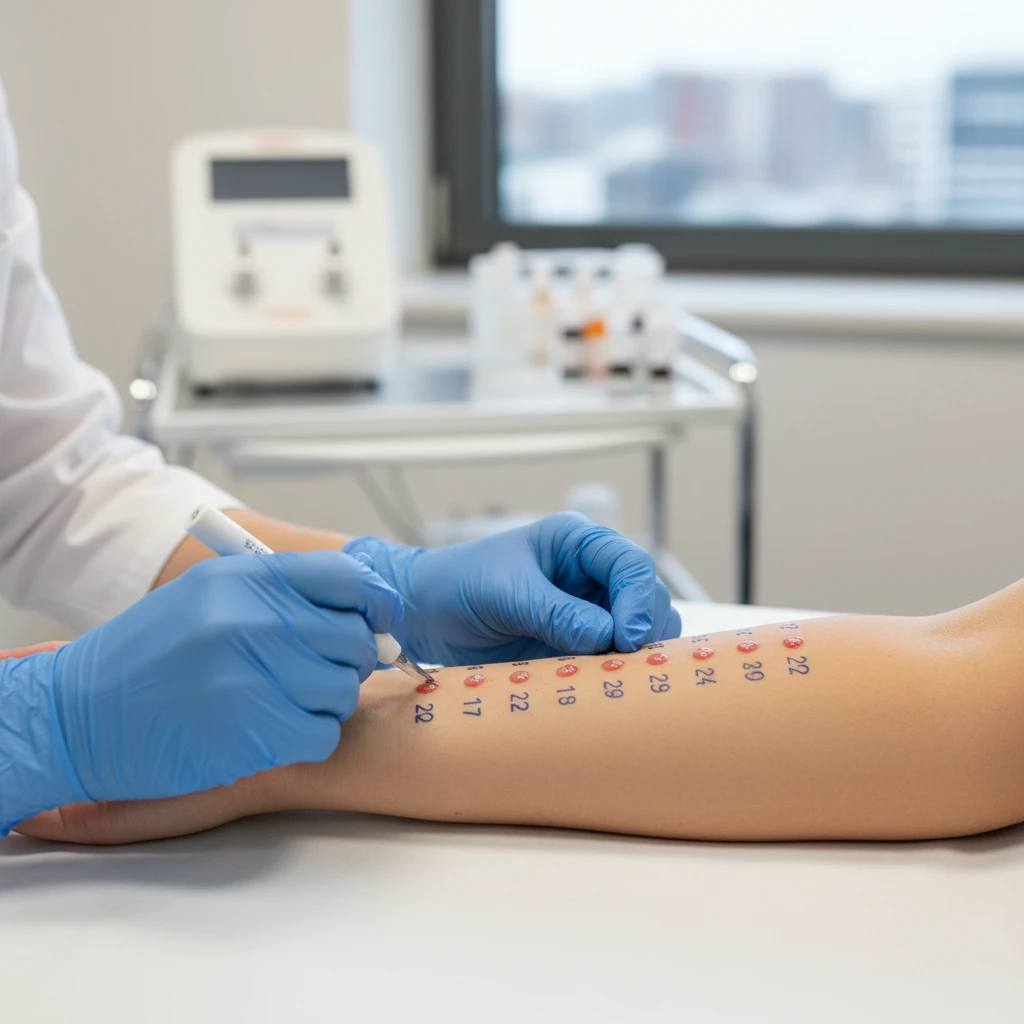
For allergies, the gold standard involves skin prick testing (SPT) conducted by an allergist. A tiny amount of the allergen is introduced to the skin; if a raised bump (wheal) appears, it indicates sensitization. Blood tests (measuring specific IgE antibodies) are also used but must be interpreted in the context of clinical history, as false positives are possible.
Elimination Diets
For intolerances, there are fewer validated medical tests. The most effective diagnostic tool is often an elimination diet followed by a controlled reintroduction challenge. This involves removing suspected triggers for 2-6 weeks until symptoms resolve, then reintroducing them one by one to identify the culprit.
Beware of Unproven Tests
Consumers should be wary of home testing kits sold online, such as IgG food sensitivity tests or hair analysis. Many major medical organizations state that these tests lack scientific validity and often lead to unnecessary dietary restrictions.
The Celiac Distinction: Autoimmune vs. Intolerance
It is vital to address Celiac Disease separately. It is frequently misclassified by the public as a severe gluten intolerance or a wheat allergy, but it is neither. Celiac disease is a serious autoimmune disorder. When a person with Celiac disease ingests gluten (a protein found in wheat, rye, and barley), their immune system attacks the lining of their own small intestine.
Unlike an intolerance, this damage causes malabsorption of nutrients and can lead to long-term health complications like osteoporosis, infertility, and neurological issues. Unlike an allergy, it does not cause anaphylaxis. The treatment, however, is strict, lifelong adherence to a gluten-free diet.
Management and Treatment Strategies
Once a diagnosis is confirmed, management focuses on avoidance and preparedness.
Managing Allergies
Strict avoidance is the primary strategy. Individuals with diagnosed food allergies must become experts at reading labels. In the United States and EU, laws require clear labeling of major allergens.
- Emergency Medication: Patients at risk of anaphylaxis must carry an epinephrine auto-injector (e.g., EpiPen, Auvi-Q) at all times.
- Immunotherapy: Oral Immunotherapy (OIT) is an emerging treatment where patients are given gradually increasing amounts of an allergen to build tolerance. This should only be done under strict medical supervision.
Managing Intolerances
Management of intolerances is often more flexible. Many people can tolerate small amounts of the trigger food.
- Enzyme Replacements: Over-the-counter lactase pills can help those with lactose intolerance consume dairy. Similar enzymes exist for bean digestion (alpha-galactosidase).
- Dietary Modification: Substituting trigger foods with alternatives (e.g., almond milk instead of cow’s milk) is the most common approach.
Living with Dietary Restrictions
Navigating daily life with allergies or intolerances requires vigilance, particularly when dining out or traveling. Cross-contact (often called cross-contamination) occurs when an allergen is inadvertently transferred from one food to another. For someone with a severe peanut allergy, a knife used for peanut butter and then wiped on a cloth before cutting a sandwich can be deadly.
Communication is key. When dining out, always inform the server and the chef of your restrictions. Use “chef cards” that clearly list your allergens in the local language when traveling. The psychological burden of these conditions is real; anxiety regarding food safety is common, and seeking support from patient advocacy groups can be beneficial.
When to See a Specialist
If you experience symptoms such as swelling of the lips or tongue, difficulty breathing, or widespread hives after eating, seek emergency medical attention immediately. For chronic digestive issues, persistent eczema, or suspected reactions to foods, consult a board-certified allergist or gastroenterologist. According to the Mayo Clinic, accurate diagnosis is the first step toward effective management and preventing unnecessary dietary restrictions.

People Also Ask
What is the main difference between an allergy and an intolerance?
The main difference is the body system involved. An allergy triggers the immune system and can be life-threatening, while an intolerance affects the digestive system and causes discomfort but is generally not fatal.
Can you suddenly develop allergies or intolerances as an adult?
Yes, adult-onset allergies and intolerances are possible. You can develop a reaction to a food you have eaten your entire life without issues due to changes in the immune system or enzyme production levels.
How long does it take for food intolerance symptoms to show?
Food intolerance symptoms typically appear anywhere from 30 minutes to 48 hours after consuming the trigger food, making them harder to diagnose than immediate allergic reactions.
Is there a cure for food allergies?
There is currently no permanent cure for food allergies. However, therapies like Oral Immunotherapy (OIT) can help desensitize the immune system, and some children may outgrow allergies to milk, eggs, soy, and wheat.
What are the symptoms of gluten intolerance vs. celiac disease?
Both cause digestive distress, but Celiac disease is an autoimmune condition that damages the small intestine and causes long-term health risks. Non-celiac gluten sensitivity causes symptoms without the intestinal damage.
Are food sensitivity tests accurate?
Most at-home food sensitivity tests (measuring IgG antibodies) are not considered accurate or clinically valid by major allergy organizations. They often reflect recent food intake rather than a true intolerance.
